Launched in October 2020 the Health Economics Unit supports health system and industry leaders to make evidence-based decisions when it comes to designing services to best meet the needs of their communities. Business Manager Tim Shaw reflects on the achievements of the first six months.
We were amid a global pandemic not to mention a national lockdown when I joined the team in January 2021 and even though we’ve set up remotely we’ve still been agile in responding to clients’ needs. We have managed to scale up quickly and demand for our expertise has made it necessary to expand the team, attracting talent from all over the UK.

The breadth of work we have undertaken has been wide ranging. While most of our work is within the public sector – mainly NHS organisations on a local and national level – we’ve also worked with the pharmaceutical industry, small medtech companies and academia, as well as collaborating with our hosts, Midlands and Lancashire Commissioning Support Unit.
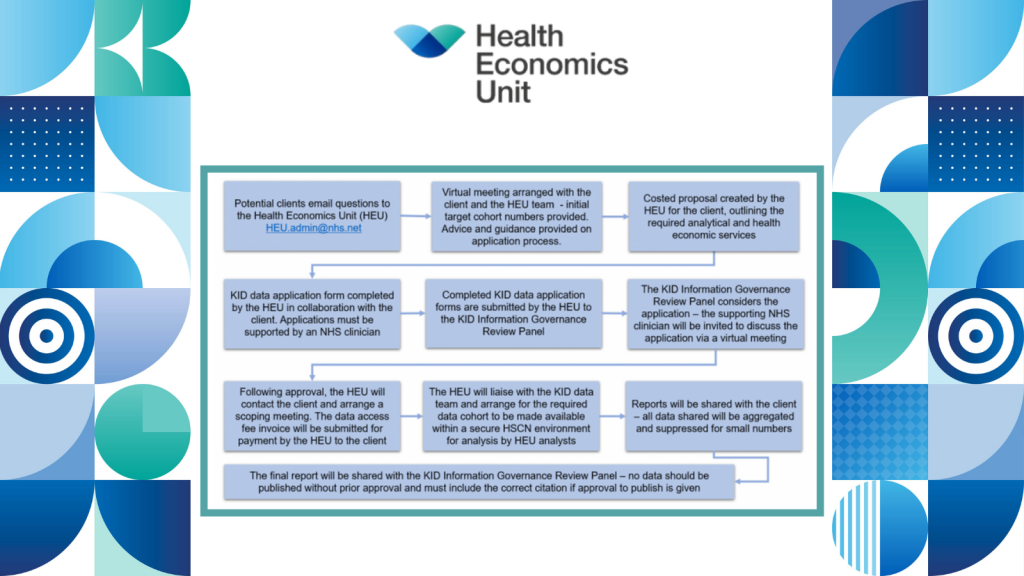
In order to support our clients we have access to a wide range of datasets such as SAIL, which covers Wales, WSIC, which covers North West London and the Kent Integrated Dataset (KID). This means we can access a wide range of rich data which we use depending on our client need. For example, the KID brings together information from GPs, NHS trusts and social care and links with criminal justice, giving deeper insight throughout a person’s lifetime.
The essence of what we do is collaborative working. It’s important we make sure we have a whole world view and are not siloed in one particular area. Using the skills we have, alongside working collaboratively with other partners, allows us to answer our client’s needs and provide a robust response.
Here are a few highlights from our first six months:
Providing analytical support for the 40 new hospitals programme
The Department of Health and Social Care is working on a national programme to build at least 40 new hospitals.
In collaboration with the Strategy Unit we’re providing analysis of the size and remit for each hospital to ensure they’re fit for purpose and the needs of the local community.
We’ll be holding workshops with local and national planning teams and developing guidelines, standards and frameworks to strengthen local and national demand forecasting capability.
Once we have a national methodological framework we will deliver a training programme to make sure all the teams involved understand how to apply these.
Ultimately this will allow for a standardised approach across the UK based on the most relevant information.
Health Economics Unit and Strategy Unit appointed to support New Hospitals Programme
Building the first national impactibility model for NHS England
We’ve been commissioned by NHS England to develop a tool that will be freely available within the NHS to provide evidence-based predictions and actionable results. This will help users model the outcome of an intervention or course of action.
It will be for use with the National Commissioning Data Repository dataset which is managed by NHS England’s data services and will support the NHS in implementing population health management in service recovery and redesign. An added benefit is that it can be modified and updated giving analysts the ability to add their own integrated data.

It’s hugely exciting to think the NHS will have access to such a powerful decision-making tool at a local level. This will really support the NHS Long Term Plan which puts much weight on population health management to improve health and wellbeing.
Join us for impactibility workshop
NHSX Accelerated Access Collaborative AI evaluations
Another collaboration with the Strategy Unit sees us working with the clinical trials units at the University of Leicester and Keele University to assess the safety, effectiveness and impact of two artificial intelligence products from the Artificial Intelligence in Health and Care Awards.
Technologies include a mobile app and home test kit for kidney disease and another supporting the early detection of diabetes-related eye disease.
The award is run by the Accelerated Access Collaborative in partnership with NHSX and the National Institute for Health Research. We’re carrying out a robust evaluation using real-world perspectives and following NICE appraisal processes to ensure the most promising AI technologies are recommended for adoption across the NHS.
Evaluating Artificial Intelligence: a significant new win.
Health economics training for pharmacists
One of our first international projects was providing health economics training in the Gulf. We have created an entire curriculum to strengthen health economics expertise and the use of decision modelling in healthcare for pharmacists in the Gulf.
The training is delivered remotely in a modular format and covers everything from why we should apply economics to healthcare through to using Excel and how to interpret data.
Providing pharmacists with this knowledge empowers them to make the best decisions by understanding the relative costs and benefits of alternative options.
This type of training can be adapted for use with other healthcare workforces.
Looking to the future
The COVID-19 pandemic has led to the most challenging time in NHS history. It’s no surprise given the current pressures facing the health service that attention needs to be given to forward planning and making sure resources are spent effectively, efficiently and in the right places. Being savvy with evidence-based decision making has an impact on the wider health system and directly improves patient care and outcomes.
We’re delighted to be expanding our team with seven new team members over the next few months and we are always looking to work with sharp, nimble and kind people that can join us and support our growth.
The Health Economics Unit continues to provide intelligence on understanding unmet needs and how resources are best used to address them. If you are interested in keeping up to date with our latest news then please follow us on Twitter and Linkedin.
 Author – Tim Shaw
Author – Tim Shaw
Tim Shaw brings a little bit of magic to the work of the Health Economics Unit.
When he isn’t managing the business side of things Tim is also a skilled and experienced manager with proven record of successful leadership and delivery of programmes in healthcare quality improvement.